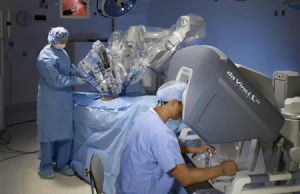
Robotic hysterectomy uses a robot to assist a surgeon to perform a laparoscopic hysterectomy. Consequently, the benefits of minimally invasive surgery are similar including less postoperative pain, tissue trauma, blood loss, and scarring; as well as a faster return to normal activities, compared to a more traditional open, abdominal hysterectomy. That is a good development for patient care. However, the reality is it takes an additional 45 minutes under anesthesia to set up the robot, costs the patient thousands of dollars in fees, and ironically does not eliminate an assistant surgeon. Despite the compelling marketing hype by many hospitals and physicians trying to recoup their multi million dollar investment, there really are no additional benefits:
Robotic Hysterectomy = Laparoscopic Hysterectomy
| Robotic Laparoscopic Hysterectomy | Laparoscopic Hysterectomy | |
| Operation Time | Longer to set up robot assistant | Faster |
| Pain | Same | Same |
| Recovery Time | Same | Same |
| Risks | Same | Same |
| Cost | Thousands More | Less |
In 2013, the American College of Obstetricians & Gynecologists published an official statement that there are really no additional benefits (except for cancer surgery) of robotic assisted hysterectomy.
Laparoscopic Supracervical Hysterectomy (LSH), where only the uterus is removed is truly redefining hysterectomy. LSH is a partial hysterectomy that preserves your cervix, and often your ovaries, removing only the diseased uterus. It offers the shortest, least painful recovery. Laparoscopic hysterectomy (including the removal of the cervix) is also an option for those women who need or prefer it. Few surgeons are trained to perform these advanced procedures. In fact, Dr. Scott Kramer was among the first (over a decade ago) to perform them in the San Francisco Bay Area.
Click here to learn more about Laparoscopic Hysterectomy
So why not simply seek a gynecologist who is experienced, skilled laparoscopic surgeons?